Hypomania vs. Mania: Understanding the Key Differences
Understanding the difference between hypomania vs. mania is essential for accurate diagnosis, effective treatment, and improved self-awareness. The symptoms can look similar, but the severity, duration, and impact on daily functioning are significantly different.
What Is Mania?
Mania is a distinct period of abnormally elevated, expansive, or irritable mood, accompanied by persistently increased energy or activity. It is a defining feature of Bipolar I Disorder.
According to the Diagnostic and Statistical Manual of Mental Disorders (DSM-5-TR), a manic episode:
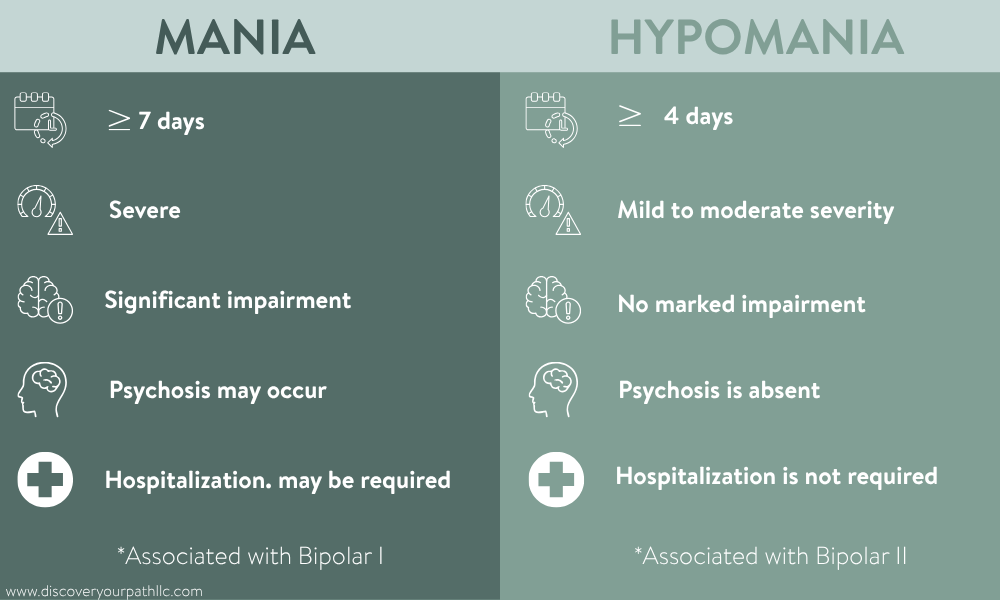
Lasts at least 7 days, or any duration if hospitalization is required
Is present most of the day, nearly every day
Causes marked impairment in social, occupational, or daily functioning
May include psychotic features, such as hallucinations or delusions
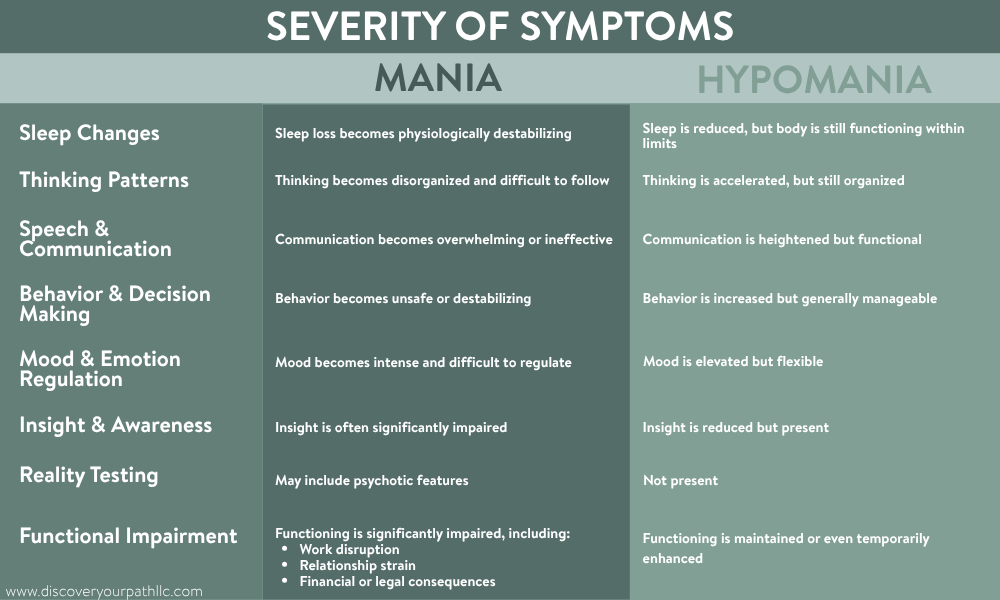
Symptoms of Mania
Common clinical features include:
Decreased need for sleep (e.g., feeling rested after only a few hours)
Inflated self-esteem or grandiosity
Increased talkativeness or pressured speech
Racing thoughts or flight of ideas
Distractibility
Increased goal-directed activity or psychomotor agitation
Engagement in high-risk behaviors (e.g., excessive spending, unsafe sexual activity, substance use)
Mania often results in significant disruption to functioning and may require urgent clinical intervention.
What Is Hypomania?
Hypomania involves similar symptoms but is less severe than mania and does not cause the same level of impairment. It is a defining feature of Bipolar II Disorder.
Per DSM-5-TR criteria, a hypomanic episode:
Lasts at least 4 consecutive days
Is observable by others as a change in functioning
Does not cause marked impairment in social or occupational functioning
Does not include psychotic features
Does not require hospitalization
Symptoms of Hypomania
Symptoms may include:
Elevated or irritable mood
Increased energy and activity
Reduced need for sleep (with less impairment than mania)
Increased confidence or goal-directed behavior
Greater sociability or talkativeness
Although hypomania may feel subjectively positive, it still represents a noticeable shift from a person’s baseline functioning and can be part of a broader mood pattern.
Why This Distinction Is Important
1. Diagnostic Clarity
Differentiating between hypomania and mania is critical for diagnosis:
Mania → Bipolar I Disorder
Hypomania → Bipolar II Disorder (when paired with depressive episodes)
Accurate diagnosis informs treatment planning, including medication and psychotherapy approaches.
2. Level of Risk
Mania is associated with greater clinical risk, including:
Impaired judgment and decision-making
Financial or legal consequences
Relationship disruption
Increased likelihood of hospitalization
Potential for psychosis
While hypomania is less severe, it can still contribute to long-term instability, particularly when followed by depressive episodes.
Causes and Contributing Factors
Research suggests that both hypomania and mania arise from a combination of biological and environmental factors, including:
Genetic predisposition
Neurochemical imbalances (e.g., dopamine dysregulation)
Circadian rhythm disruption (especially sleep deprivation)
High stress or significant life changes
Substance use
Certain medications (e.g., antidepressants in some individuals)
When to Seek Professional Support
It may be helpful to consult a licensed mental health professional if you or someone you know experiences:
Noticeable and sustained changes in mood or energy
Decreased need for sleep without fatigue
Impulsive or uncharacteristic behaviors
Cycles of elevated mood followed by depression
Feedback from others expressing concern about behavioral changes
Early assessment can support accurate diagnosis, symptom management, and improved long-term outcomes.
Recognizing the differences of hypomania vs. mania is essential for understanding mood patterns and accessing appropriate care. The symptoms may look the same. The severity and impairment is the key difference.